Radiation Oncology
Milestones in Radiation Oncology at NCT Heidelberg
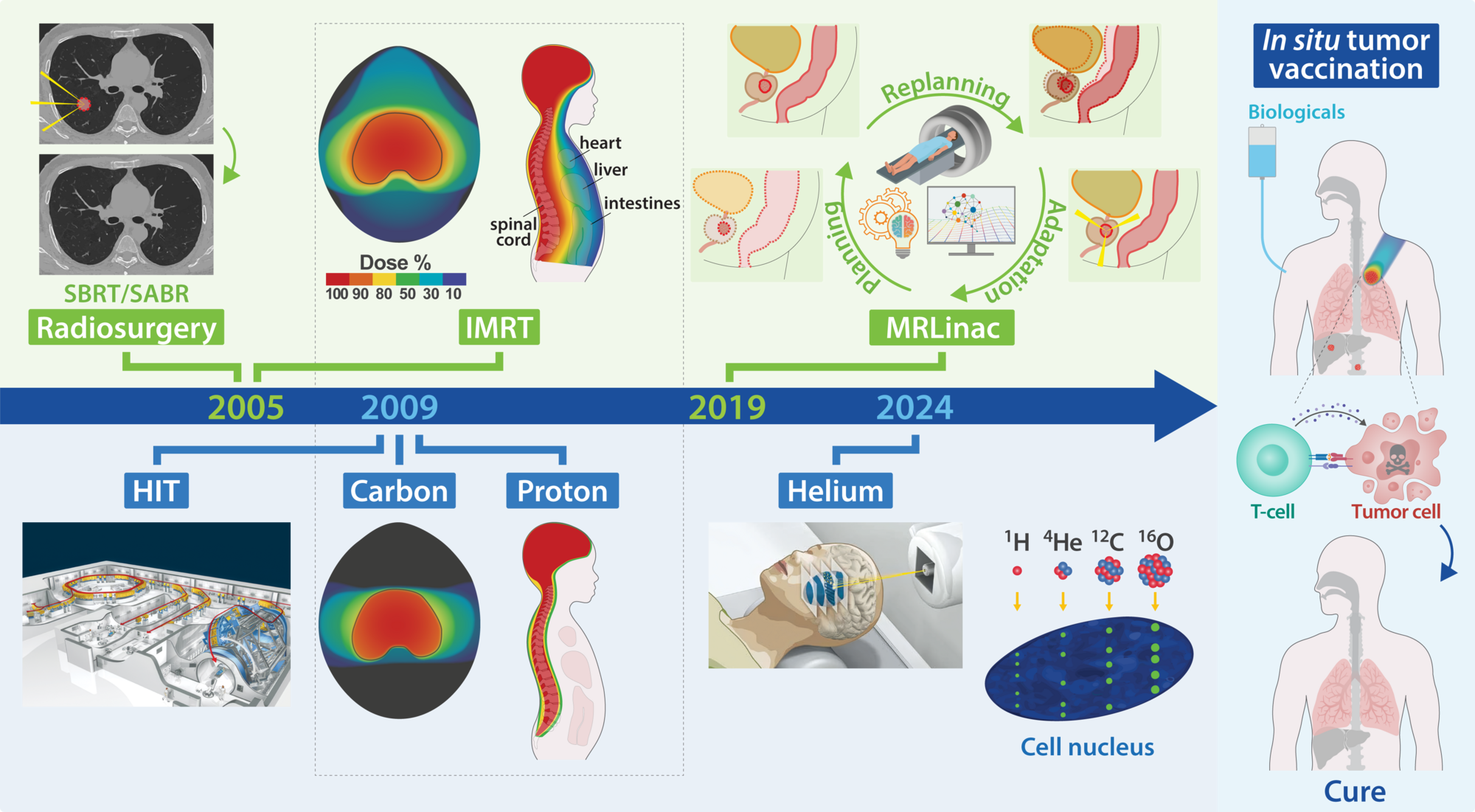
Over the past two decades, the Department of Radiation Oncology at NCT Heidelberg has become an internationally recognized center for research and innovation. Heidelberg scientists have played a major role in developing intensity-modulated radiotherapy (IMRT) and stereotactic body radiotherapy/radiosurgery (SBRT/SABR), setting new standards for precise cancer treatments from which many patients benefit today.
Since 2019, the integration of modern magnetic resonance imaging (MRI) into the linear accelerator (MR-Linac) has enabled real-time tracking of tumors and surrounding organs during treatment. Combined with artificial intelligence, radiotherapy can now be adapted instantly, allowing tumors to be targeted more precisely while sparing healthy tissue and often reducing the number of treatment sessions.
At the Heidelberg Ion-Beam Therapy Center (HIT), interdisciplinary research exploits the unique properties of different ion species – currently protons, helium, carbon, and oxygen ions – for new treatment options. Proton therapy is now a standard of care for many solid tumors in children, due to its tissue-sparing properties. Heavier particles such as helium and carbon ions scatter less than protons, making them particularly well suited for deep-seated tumors located near critical structures, such as skull base tumors.
While the physical limits of precision radiotherapy are being reached, new insights into the biological effects of ion beams open promising opportunities. Combining particle therapy with molecular and immunological approaches may help overcome tumor resistance and reshape the tumor microenvironment. One future vision is in situ tumor vaccination, where particle therapy could reprogram tumors in a way that activates the patient’s own immune system, leading to more effective and gentler cancer treatments.