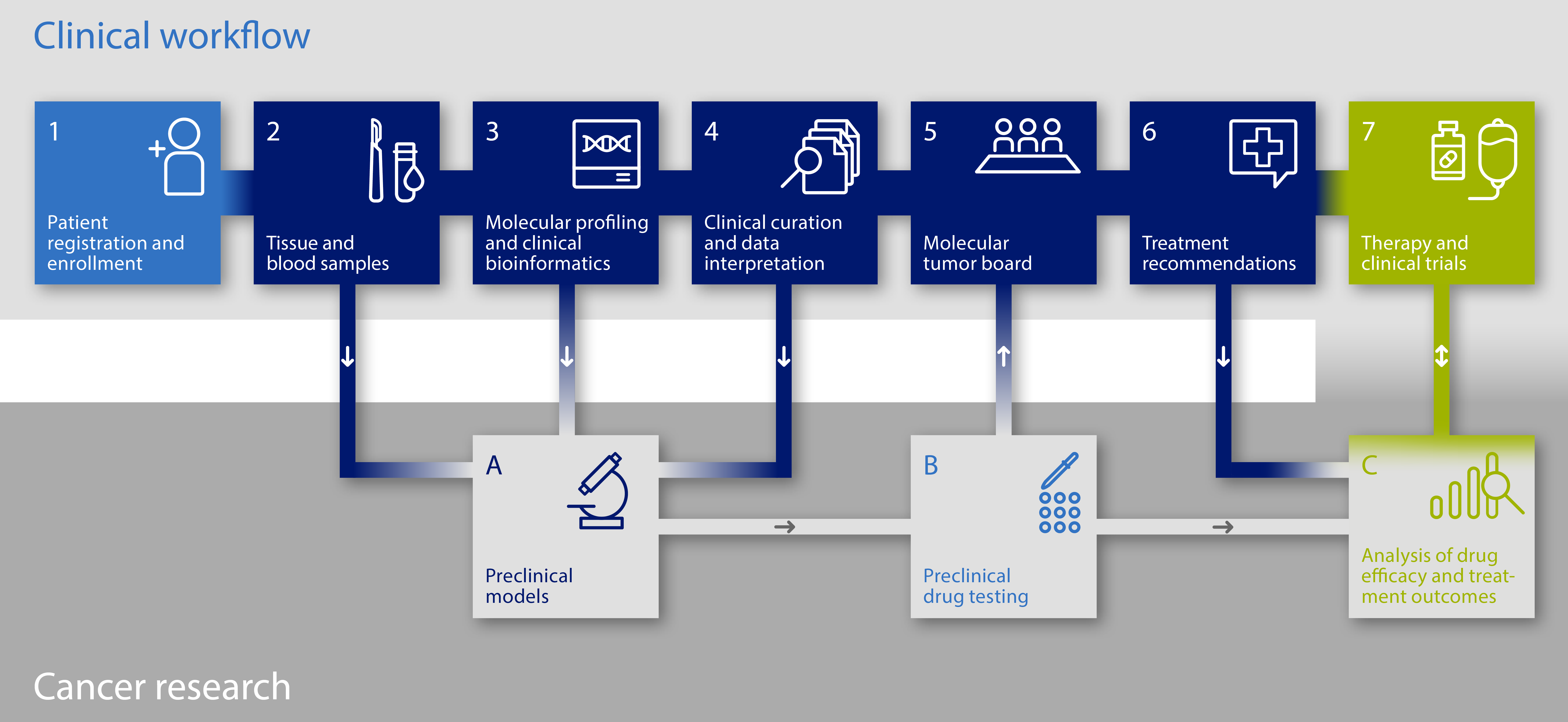
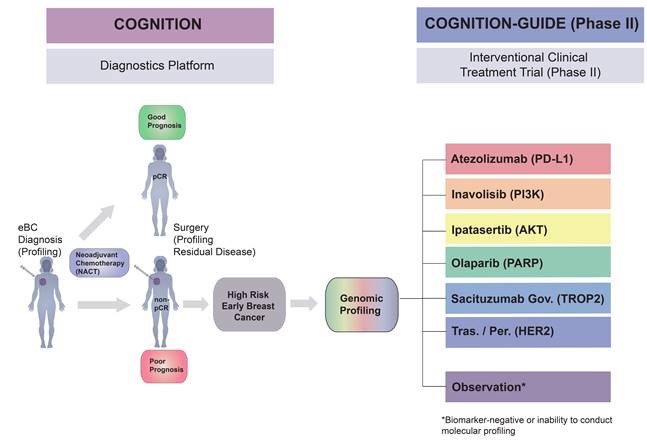
The diagnostic platforms follow a standardised workflow:
1. Information / enrolment at the NCT Heidelberg or any other participating study center
2. Acquisition of biomaterial (tissue + blood) for molecular analyses in the course of standard routine procedures or as a study specific measure
- Tumor tissue: Fresh tissue samples (no FFPE if possible) as pre-requesite for downstream molecular-genetic analyses
- Blood withdrawal (comparative sample of normal body cells to define tumor-specific genetic alterations)
3. Evaluation tumour cell content fresh tissue sample (minimum content 20 % tumor cells) and tumor infiltrating lymphocytes
4. Molecular Analyses: Tumor-Genome-Sequencing (DKFZ Heidelberg) / Next Generation Sequencing
- Analyte-Isolation (DNA, RNA, Protein, Sample Processing Lab, DKFZ)
- Sample preparation for high-throughput sequencing (Genomics Core Facility, DKFZ)
- Method: whole-genome/ whole-exome and transcriptome sequencing
5. Discussion of molecular-genetic findings within the interdisciplinary molecular tumor board
- Participants: Oncologists, bioinformaticians, molecular biologists, pathologists, human geneticists
- Prioritisation of therapy-relevant gene alterations and molecular targets
- Generating a therapy plan combined in a molecular report
6. Discussion of molecular-genetic findings and consideration of possible treatment options with the patient
7. Biomarker-based, personalised treatment with targeted substances according to the genetic tumor profile at the NCT Heidelberg (outside the Register study) in a prospective 9-armed Phase II treatment study (COGNITION-GUIDE), which is planned for the beginning of 2021.